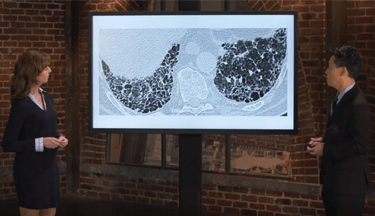
Interstitial Pneumonia with Autoimmune Features
OVERVIEW
An estimated 25% of patients with suspected systemic rheumatic disease have symptoms that point to underlying autoimmunity but do not have enough features that result in a clear diagnosis of connective tissue disease (CTD).1,2 IPAF is a term to identify patients who have idiopathic interstitial pneumonia and features consistent with a CTD but do not fit criteria suggestive of a definitive CTD diagnosis.3
CLASSIFICATION CRITERIA3
Classification criteria for an IPAF diagnosis surrounds the presence of a combination of features from three domains:
CLINICAL DOMAIN3
- Extra-thoracic clinical features
- Mechanic’s hands
- Digital tip ulceration
- Inflammatory arthritis
- Palmar telangiectasia
- Raynaud’s phenomenon
- Digital edema
- Gottron’s sign
SEROLOGIC DOMAIN3
- Specific autoantibodies including:
- ANA (Antinuclear antibody)
- Rheumatoid factor
- Anti-CCP (cyclic citrullinated peptide)
- Anti-Ro/La (SS-A)/(SS-B)
- Anti—ribonucleoprotein
- Anti-topoisomerase (Scl-70)
- Anti-tRNA synthetase (e.g. Jo-1, PL-7, PL-12; others)
- Anti-PM-Scl (polymyositis scleroderma)
- Anti-MDA-5 (melanoma differentiation-associated protein 5)
MORPHOLOGIC DOMAIN3
- High resolution computed tomography (HRCT), histopathologic, or physiologic pulmonary features
- HRCT/Histopathology
- NSIP (non-specific interstitial pneumonia)
- OP (organizing pneumonia)
- Non-specific interstitial pneumonia/organizing pneumonia (NSIP/OP)
- LIP (lymphoid interstitial pneumonia)
- HRCT/Histopathology
- Other Histopathology
- Multicompartment involvement