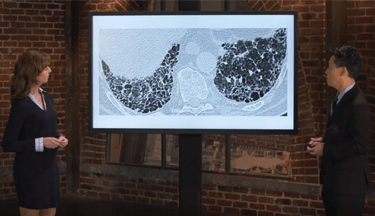
Exposure-related ILD
Overview
Exposure-related ILDs are responsible for 20% of all ILDs.1 These ILDs impact individuals of all ages, with the causative agent often differing between adults and children.2
- Exposure-related pediatric ILD is thought to be underestimated2
- Misdiagnosis or underestimation of pediatric ILD often leads to diagnosis when the disease is already chronic2
- Most cases of pediatric ILD are due to environmental or avocational hypersensitivity pneumonitis, radiation exposure, or are drug induced2
- Adults are often exposed within the workplace1
DRUG-ASSOCIATED ILD3
- Drug-induced lung injury can involve multiple parts of the lung:
- Airways
- Lung parenchyma
- Mediastinum
- Pleura
- Vasculature
- Neuromuscular system
- Most common form is ILD
- Route of drug administration associated with ILD is often oral or parenteral, but can also be from nebulized or intrathecal medication
- Direct (often seen with chemotherapeutics) or indirect actions of certain drugs can lead to ILD
CAUSATIVE AGENTS
Over 450 drugs from a variety of classes have been associated with ILD:3
- Cytotoxic (e.g., bleomycin, carmustine, busulfan, cyclophosphamide)3
- Cardiovascular (e.g., amiodarone, statins)2,3
- Anti-inflammatory or immunosuppressive (e.g., aspirin, methotrexate, azathioprine, NSAlDs)2,3
- Antibiotics or antimicrobials (e.g., nitrofurantoin, amphotericin B, sulfonamides, sulfasalazine)2,3
- Biological agents (e.g., tumor necrosis factor-α (TNF-α) blockers, anti-CD20 antibodies, interferon-α (INF-α)3
- Miscellaneous (e.g., bromocriptine)3
EPIDEMIOLOGY3
- An estimated 2.5%-3% of ILD cases are thought to be drug-induced
- ILD is most commonly found among patients exposed to known ILD—causing agents, particularly in populations such as:
- Patients receiving chemotherapy
- Patients with inflammatory conditions such as rheumatoid arthritis or inflammatory bowel disease
- Patients receiving concurrent toxic therapeutic agents
DISEASE PROGRESSION4
Drug-specific pathways:
- With chemotherapeutics, the release of cytokines is directly related to the causative drug and can cause capillary leakage and pulmonary edema
- Methotrexate-associated ILD is thought to induce release of free oxygen radicals
- A similar mechanism may underlie bleomycin, nitrofurantoin, and mitomycin C-induced ILD
- The lung is particularly sensitive to bleomycin toxicity as the drug is preferentially distributed to the lung, and has lower levels of the detoxifying enzyme
- A similar mechanism may underlie bleomycin, nitrofurantoin, and mitomycin C-induced ILD
- Gefitinib impairs alveolar repair mechanisms and impacts epithelial proliferation underlying pulmonary fibrosis
- Amiodarone disrupts lysosomal membranes, leading to release of oxygen radicals and the activation of caspase-mediated apoptosis in lung epithelial cells
RISK FACTORS
General Risk Factors3
- Age
- Children and the elderly are associated with a higher risk3
- Gender
- Higher incidence in females3
- Ethnicity
- Dosage
- Oxygen
- Drugs inducing reactive oxygen species and oxidative stress may contribute to ILD3
- Drug interactions
- Certain drug combinations can elicit, or increase the risk of ILD3
- Radiation
- Underlying drug disease
Risk for Immune Reactions4
- Drug structure
- Genetics
- Environment
- Nature of drug exposure